How does the brain rid itself of waste, and how does this process influence our health? In a landmark study led by researchers at Washington University in St. Louis and the National Institute of Neurological Disorders and Stroke, scientists have uncovered a direct pathway through which the brain’s waste disposal system communicates with the protective layers surrounding it, challenging long-standing beliefs about the brain’s isolation from the body’s immune system.
This discovery sheds light on the mechanisms that allow waste and immune signals to move between the brain and its outer protective covering, potentially opening new avenues for understanding and treating neurological diseases. The findings have been published in the journal Nature.
The motivation behind this study stems from a fundamental question in neuroscience: how does the brain, an organ known for its delicate and complex functions, maintain its health by removing waste and interacting with the body’s immune system? Traditionally, the brain was thought to operate in a sort of splendid isolation, protected by barriers that keep out the immune system and potentially harmful substances.
However, this isolation could also mean that the brain had limited options for waste removal, a critical function for preventing diseases. Researchers embarked on this study to explore the possibility of a direct communication route between the brain and its surrounding protective layers, which could revolutionize our understanding of brain health and disease.
“Waste fluid moves from the brain into the body much like how sewage leaves our homes,” said Daniel S. Reich, a senior investigator at NINDS. “In this study, we asked the question of what happens once the ‘drain pipes’ leave the ‘house’ — in this case, the brain — and connect up with the city sewer system within the body.”
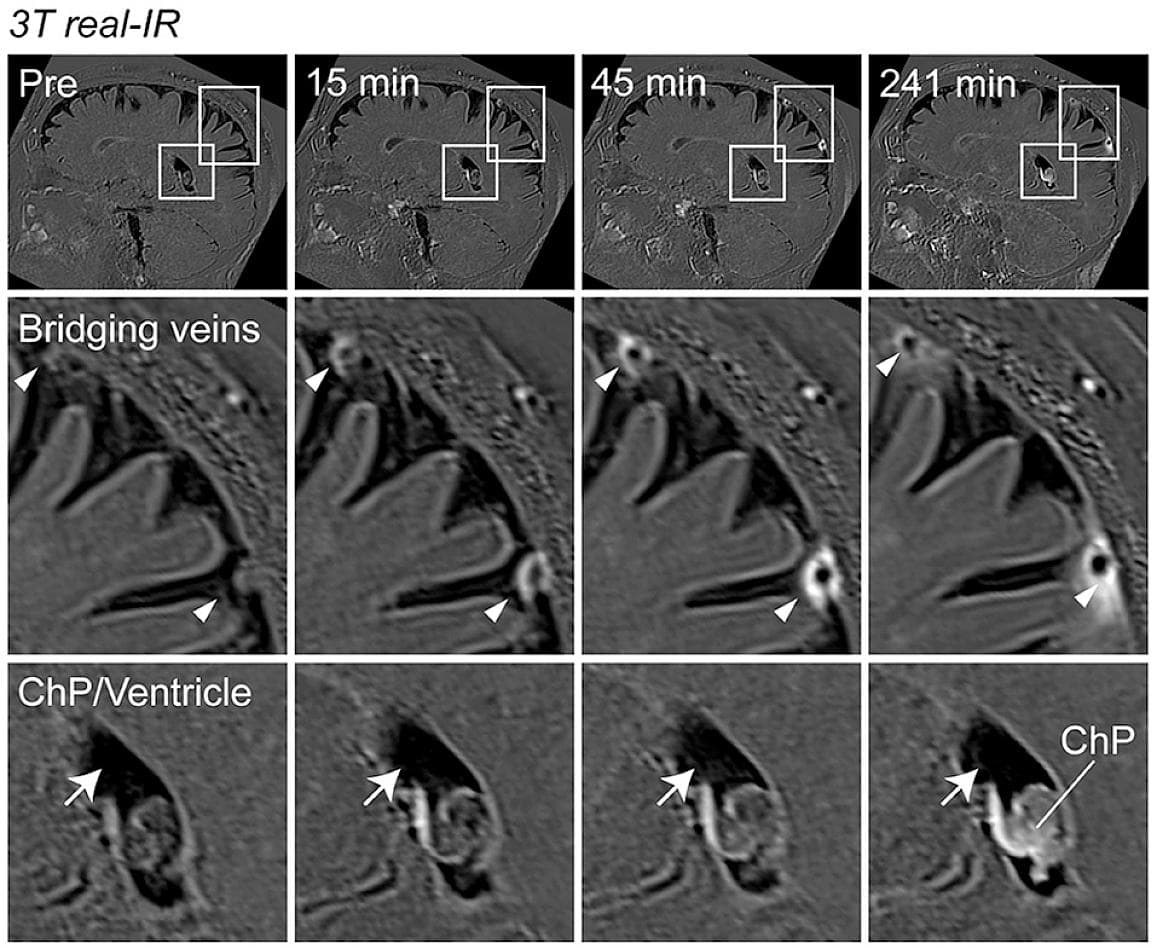
To investigate these questions, the study employed a comprehensive approach combining advanced imaging techniques and genetic analysis in both humans and mice. In humans, the team used high-resolution magnetic resonance imaging (MRI) to observe the movement of a magnetic dye, gadobutrol, which was injected into participants to visualize the pathways through which waste might exit the brain.
In parallel, researchers conducted experiments in mice, injecting them with light-emitting molecules to track the movement of fluids through the brain’s protective barriers. The study also utilized single nucleus RNA-sequencing to analyze the gene expression of cells within these barriers and electron microscopy to visualize the cells’ structures in detail.
The researcher identified specific regions, termed arachnoid cuff exit (ACE) points, where a “cuff” of cells surrounds blood vessels as they pass through the brain’s protective arachnoid barrier into the dura mater. The dura mater is the outermost and toughest layer among the three layers of membranes called the meninges that surround and protect the brain and spinal cord. This membrane is composed of dense, fibrous connective tissue.
These ACE points act as gateways, allowing the transfer of waste fluids, immune cells, and other molecules between the brain and the dura, contrary to the previous belief that such communication was virtually impossible due to the brain’s protective barriers.
This discovery reveals that the brain is not as isolated as once thought and has a direct means of disposing of waste and interacting with the immune system.
“If your sink is clogged, you can remove water from the sink or fix the faucet, but ultimately you need to fix the drain,” explained Jonathan Kipnis, a professor at Washington University in St. Louis. “In the brain, clogs at ACE points may prevent waste from leaving. If we can find a way to clean these clogs, it’s possible we can protect the brain.”
In mice, the study showed that these pathways are involved in the immune system’s response to disorders, such as when immune cells attack the brain’s protective myelin in conditions mimicking multiple sclerosis. Blocking the interaction of immune cells with the ACE points reduced the severity of the condition, highlighting the significance of these pathways in brain health and disease.
“The immune system uses molecules to communicate that cross from the brain into the dura mater,” said Kipnis. “This crossing needs to be tightly regulated, otherwise detrimental effects on brain function can occur.”
The researchers also noted that the efficiency of these ACE points and their role in waste clearance and immune surveillance might decline with age. This was suggested by the observation that older participants in the study showed increased leakage of the magnetic dye into the surrounding fluid and spaces around the blood vessels, indicating a potential breakdown in the efficiency of these ACE points over time.
This aspect of the study hints at a possible link between the aging process and the increased risk of developing neurological diseases, suggesting that the deterioration of these ACE points could contribute to the accumulation of waste products and altered immune responses in the aging brain.
“This might point to a slow breakdown of the ACE points over the course of aging,” said Reich, “and this could be consequential in that the brain and immune system can now interact in ways that they’re not supposed to.”
The discovery of ACE points revolutionizes our understanding of brain physiology, indicating a direct pathway for waste disposal and immune system interaction that was previously unknown. But he study is not without its limitations. The exact mechanism by which these ACE points operate and their relative importance compared to other waste removal and immune system interaction pathways in the brain remains unclear. Furthermore, while the study provides compelling evidence in mice and through MRI imaging in humans, more research is needed to fully understand the implications of these findings for human health and disease.
Future research directions include exploring how the efficiency of these ACE points changes with age, as the study observed increased leakage of the magnetic dye in older participants, suggesting that the effectiveness of this waste disposal system may decline over time. This could have profound implications for understanding age-related neurological diseases, where impaired waste clearance could play a critical role.
The study, “Identification of direct connections between the dura and the brain,” was authored by Leon C. D. Smyth, Di Xu, Serhat V. Okar, Taitea Dykstra, Justin Rustenhoven, Zachary Papadopoulos, Kesshni Bhasiin, Min Woo Kim, Antoine Drieu, Tornike Mamuladze, Susan Blackburn, Xingxing Gu, María I. Gaitán, Govind Nair, Steffen E. Storck, Siling Du, Michael A. White, Peter Bayguinov, Igor Smirnov, Krikor Dikranian, Daniel S. Reich, and Jonathan Kipnis.